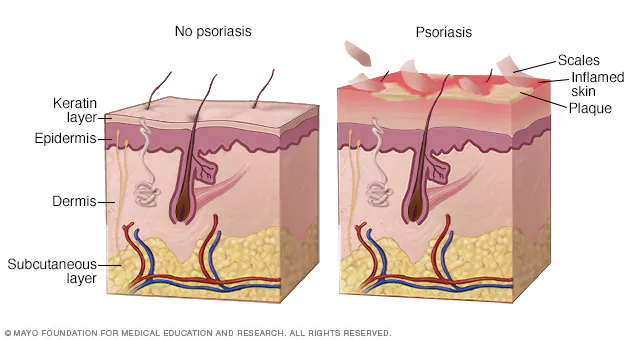
Psoriasis is one of those skin conditions that looks straightforward on the surface—red patches, scaling, itching—but underneath, it’s driven by a complex interplay of genetics, immunity, and environmental triggers. To understand why psoriasis happens, you need to look deeper than the skin. This condition isn’t caused by poor hygiene, diet mistakes, or anything someone “did wrong.” It’s a medical disorder rooted in how the body’s immune system behaves.
In this article, we break down the real reasons psoriasis develops, why it flares, who is more likely to get it, and what keeps it under control. The goal is simple: clarity, not confusion.
If you believe in this fight too, please consider supporting our mission through Donation. Together, we can make a difference.
1. Psoriasis Begins With an Overactive Immune System
The heart of psoriasis lies in immune malfunction.
In healthy skin, cells grow and shed gradually in about 28–30 days. In psoriasis, the immune system mistakenly sends inflammatory signals that make the skin multiply almost 10 times faster than normal—within 3–5 days.
The result?
- Thickened patches
- Silvery scales
- Red, inflamed skin
- Itching or burning
The body is essentially “attacking” normal skin cells, thinking it’s protecting you from a threat that doesn’t exist.
Why does the immune system do this?
Researchers point to autoimmunity. T-cells, which normally fight infections, become overactive and trigger chronic inflammation. This inflammation is what drives the rapid skin growth.
Psoriasis isn’t “just” a skin disease; it’s a long-term immune condition that shows up on the skin.
2. Genetics Play a Massive Role — Psoriasis Often Runs in Families
Genes set the stage long before symptoms appear.
If one parent has psoriasis, the risk of developing it goes up significantly. If both parents have it, the risk increases even more. But not everyone with the genes will develop symptoms. You inherit the possibility, not the guarantee.
What do genes actually do?
Certain genes involved in immune regulation can become overly active:
- They make inflammatory responses stronger
- They tell the body to produce excessive immune signals
- They increase sensitivity to triggers
This means someone may carry psoriasis-related genes for years without a flare until the “right” environmental trigger hits.
3. Triggers Activate Psoriasis in People Already Predisposed
Psoriasis doesn’t just appear out of nowhere. It usually needs a trigger. These triggers don’t cause psoriasis by themselves—they activate it if the underlying risk is already there.
Common Psoriasis Triggers
- Stress
One of the biggest drivers. Stress increases inflammatory hormones that directly worsen immune activity. - Infections
- Strep throat
- Skin infections
- Viral illness
- Skin injuries (Koebner phenomenon)
Cuts, burns, bug bites, or even tattoos can trigger new lesions. - Cold weather
Dry air and minimal sunlight reduce natural skin healing. - Smoking and alcohol consumption
Both are linked to increased inflammation in the body. - Certain medications, including:
- Beta-blockers
- Lithium
- Some antimalarials
- Steroid withdrawal
- Hormonal shifts
Puberty, pregnancy, and menopause can change flare patterns.
These triggers explain why two people with similar genetics may have completely different flare patterns.
4. Environmental and Lifestyle Factors Add Fuel to the Fire
Psoriasis doesn’t happen because of lifestyle choices, but lifestyle can worsen the immune system’s response.
Inflammation is the link
Any condition or habit that increases body inflammation can intensify psoriasis activity. Examples include:
- Chronic stress
- Poor sleep
- Obesity
- Exposure to cigarette smoke
- High inflammatory diets
Again, none of these “cause” psoriasis outright—they magnify the immune system’s overreaction.
5. The Skin Barrier Is Weaker in Psoriasis Patients
A healthy skin barrier protects the body from irritants, germs, and environmental stress. In psoriasis, this barrier is often weaker or more reactive.
Why does this matter?
- Irritants penetrate more easily
- Dryness increases
- Inflammatory reactions accelerate
- Healing takes longer
This weak barrier doesn’t cause psoriasis, but it helps explain why the condition flares aggressively once it begins.
6. Psoriasis Is Not Caused by Diet, but Diet Influences It
There is no specific food that directly causes psoriasis. But food can influence inflammation levels.
Foods that may worsen symptoms:
- Highly processed foods
- Excess sugar
- Heavy alcohol intake
- Foods high in trans fats
Foods that may support better skin health:
- Fruits and vegetables
- Omega-3–rich foods (fish, nuts, seeds)
- Whole grains
- Anti-inflammatory herbs like turmeric or ginger
Diet can’t “cure” psoriasis, but it can help reduce flare frequency for some people.
7. Hormones and Psoriasis — The Hidden Link
Hormones influence immune activity and skin cell turnover. This makes psoriasis flare or improve depending on life stages.
Examples:
- Puberty: Flares often begin here
- Pregnancy: Some women improve, some flare
- Menopause: Many women experience worsening symptoms
This shows that psoriasis is deeply connected to internal body systems, not just external factors.
8. Why Some People Develop Severe Psoriasis While Others Don’t
Severity usually depends on:
- Genetic strength
- Trigger exposure
- Immune system intensity
- Lifestyle and environmental factors
Some people only get mild patches. Others may see large areas of their body affected. It’s not about discipline or hygiene—it’s about biology.
9. Psoriasis Doesn’t Have a Single Cause — It’s Multifactorial
To summarize, psoriasis happens because:
- The immune system becomes hyperactive
- Genetics create susceptibility
- Triggers activate symptoms
- Environmental factors increase inflammation
- The skin barrier reacts more intensely than normal
These elements work together, not individually.
Final Thoughts: Understanding Psoriasis Helps You Manage It Better
Psoriasis is a long-term immune condition, not a temporary rash. Knowing why it happens helps people respond with clarity rather than confusion. You can’t change your genes or immune structure, but you can change how you manage triggers, lifestyle habits, stress, and treatment.
With proper care, psoriasis can be controlled—even if it can’t be permanently cured yet. And the more people understand the real causes behind it, the easier it becomes to manage both medically and emotionally.
NOTE: If you believe in this fight too, please consider supporting our mission through Donation. Together, we can make a difference.