Psoriasis is more than just a rash; it’s a chronic autoimmune condition that accelerates the life cycle of skin cells, leading to a rapid buildup on the skin’s surface. This can manifest in a variety of ways, making it challenging to self-diagnose. While only a dermatologist can provide a definitive diagnosis, understanding the different types of psoriasis can empower you to have a more informed conversation with your doctor.
The statistics are compelling: an estimated 125 million people worldwide live with psoriasis, impacting their physical comfort, emotional well-being, and quality of life. Knowing which type you have is the first step towards effective management and finding the right treatment path.
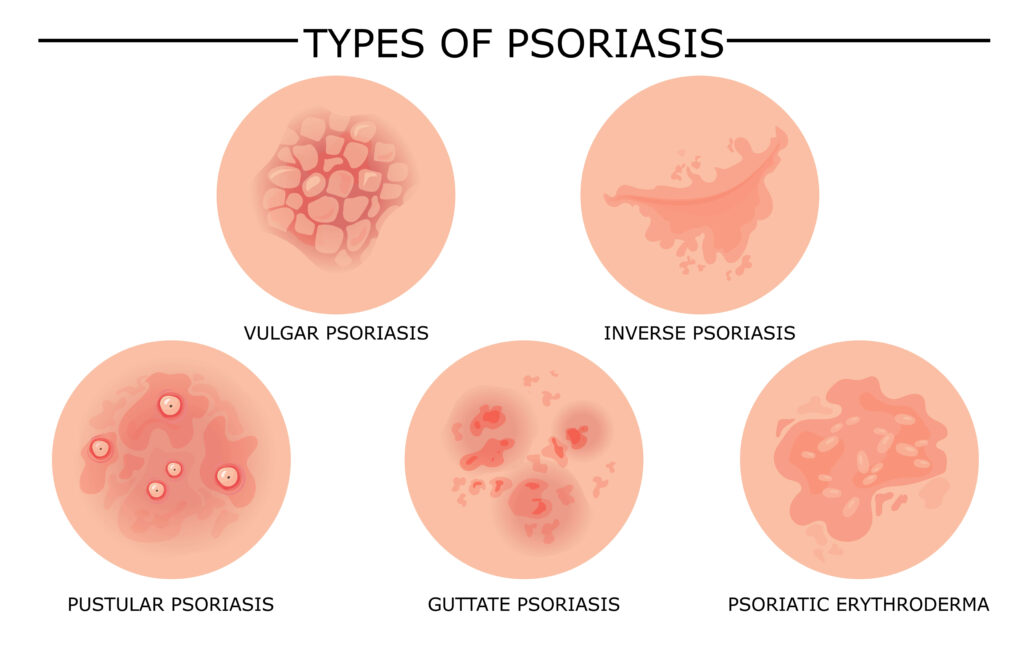
Let’s dive into the most common types of psoriasis and their distinctive characteristics:
1. Plaque Psoriasis (Psoriasis Vulgaris)
This is by far the most common form, accounting for about 80-90% of all cases. If you’re picturing psoriasis, you’re likely envisioning plaque psoriasis.
Key Characteristics:
- Appearance: Red, inflamed patches of skin covered with silvery-white scales. These plaques can be itchy and painful, sometimes cracking and bleeding.
- Location: Most commonly found on the elbows, knees, scalp, and lower back, but can appear anywhere on the body.
- Size: Can range from small, scattered patches to large areas that merge together.
- Triggers: Stress, infections (like strep throat), skin injury (Koebner phenomenon), certain medications, and even cold, dry weather can exacerbate plaque psoriasis.
What it feels like: Imagine the persistent irritation of a very dry, scaly patch that just won’t go away, often accompanied by an incessant itch that can disrupt sleep and daily activities.
2. Guttate Psoriasis
Often appearing suddenly, guttate psoriasis is the second most common type and frequently affects children and young adults.
Key Characteristics:
- Appearance: Small, red, dot-like lesions, often described as “raindrops” or “teardrops.” They are usually covered with a fine scale, but it may be less prominent than in plaque psoriasis.
- Location: Primarily seen on the trunk, arms, and legs, but can also appear on the scalp and face.
- Triggers: Most commonly preceded by a bacterial infection, particularly strep throat, about 2-3 weeks prior to the flare-up.
- Prognosis: Can sometimes clear up on its own within weeks or months, but may recur or evolve into plaque psoriasis in some individuals.
What it feels like: A sudden eruption of small, itchy spots, sometimes appearing after an illness, making you wonder if it’s a new rash or something more.
3. Inverse Psoriasis (Flexural Psoriasis)
This type of psoriasis thrives in skin folds, making it distinct from other forms.
Key Characteristics:
- Appearance: Smooth, red, inflamed patches that are often shiny and lack the characteristic scaling of plaque psoriasis due to the moist environment.
- Location: Found in skin folds such as the armpits, groin, under the breasts, and in the genital area.
- Symptoms: Can be very irritating, itchy, and painful due to friction and sweating. Fungal or yeast infections can also complicate inverse psoriasis.
- Triggers: Friction, sweating, and fungal infections can worsen symptoms.
What it feels like: A persistent, intensely red rash in sensitive areas, often mistaken for a fungal infection, causing discomfort and irritation.
4. Pustular Psoriasis
While less common, pustular psoriasis can be severe and requires immediate medical attention.
Key Characteristics:
- Appearance: Characterized by clearly defined, raised bumps (pustules) filled with non-infectious pus. The skin surrounding the pustules is typically red and tender.
- Location: Can appear in widespread patches (generalized pustular psoriasis, or GPP) or be localized to specific areas like the palms and soles (palmoplantar pustulosis).
- Symptoms: GPP can be accompanied by fever, chills, severe itching, rapid pulse, and muscle weakness, and requires emergency care.
- Triggers: Can be triggered by certain medications, infections, stress, pregnancy, or withdrawal from systemic steroids.
What it feels like: A sudden, painful eruption of pus-filled bumps on red skin, often accompanied by systemic symptoms that make you feel very unwell.
5. Erythrodermic Psoriasis
This is the least common and most severe form of psoriasis, covering nearly the entire body with a red, peeling rash. It can be life-threatening and requires immediate medical attention.
Key Characteristics:
- Appearance: Widespread, fiery red rash that covers most of the body. The skin often sheds in sheets rather than fine scales.
- Symptoms: Intense itching and pain, swelling, fever, chills, and can disrupt the body’s temperature regulation. Risk of dehydration, infection, and heart failure is high.
- Triggers: Can be triggered by a severe sunburn, infections, certain medications, or uncontrolled plaque psoriasis.
What it feels like: The feeling of your entire body being severely sunburned and peeling, accompanied by systemic symptoms that can make you feel extremely ill.
What to Do If You Suspect Psoriasis
If you’re experiencing any of these symptoms, the most crucial step is to consult a dermatologist. They will examine your skin, review your medical history, and may even perform a small skin biopsy to confirm the diagnosis.
Here’s how you can prepare for your appointment:
- Keep a symptom journal: Note when symptoms started, what they look like, where they appear, how often they flare, and any potential triggers.
- List current medications: Include both prescription and over-the-counter drugs, as some can impact psoriasis.
- Mention family history: Psoriasis often has a genetic component.
Understanding which type of psoriasis you have is fundamental to developing an effective treatment plan, which can range from topical creams and phototherapy to oral medications and biologics. With the right diagnosis and treatment, managing psoriasis and improving your quality of life is absolutely achievable.